Transplantation of the entire thickness of the cornea (penetrating keratoplasty) may be performed if there is enough normal tissue present. Several different surgical approaches may be taken, and no one approach is currently established as the standard.Įxamples of surgical procedures used for PMD include: wedge resection, lamellar crescentic resection, penetrating keratoplasty, lamellar keratoplasty, epikeratoplasty and intracorneal segments. Therefore, surgery is usually reserved for patients that do not tolerate contact lenses. There is evidence suggesting corneal collagen cross-linking may be beneficial for patients with pellucid marginal degeneration.Ĭorneal transplant surgery may be difficult due to the peripheral thinning of the cornea, even with large and off-center grafts. The use of intacs implants has been tested as a treatment for PMD, with slight improvement in visual acuity noted after eleven months,and intacs have been used with keratoconus with success. The highlight to the scleral design and the correction of eye disorders such as Pellucid Marginal Degeneration is that vision with these types of lenses is exceptional when fit correctly. Regardless of the lens size, it is thought that the larger the GP lens, regardless of the fact that it is a rigid lens, will in most cases be more comfortable then standard rigid corneal lenses, and at times more comfortable than soft lenses. Most of these lenses are in the range of 15.5mm to 18.0mm in diameter. New studies show that the use of a "GP" or Scleral contact lens has shown promise for most patients that exhibit Pellucid Marginal Degeneration. Patients wearing contacts report increased problems with glare and contrast sensitivity, but it is not clear if this is due to the corneal disease, or the contact lenses themselves. 
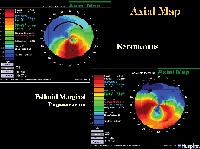
Success has been shown with the use of rigid contact lenses combined with over-refraction. Most patients can be treated non-surgically with eye glasses, or contact lenses.Įarly stages of PMD may also be managed with soft contact lenses. Thus, if corneal topography is used for diagnosis, it should be in conjunction with clinical findings of peripheral, inferior corneal thinning. However, it may not as specific as corneal pachymetry, because corneal topography only evaluates the degree and distribution of surface irregularities on the cornea, not the thickness of the cornea.Ĭorneal topography may show a "crab claw-like" appearance, a finding that is seen in both keratoconus and in pellucid marginal degeneration. The gold standard diagnostic test for PMD is corneal topography. Unlike keratoconus, PMD lacks apical corneal scarring, Rizutti's phenomenon, Munson's sign, and the central corneal thickness is usually normal. The inferior peripheral thinning is seen between the 8 o'clock and 4 o'clock positions. In PMD we can see high against the rule astigmatism along with horizontal bow ties. The portion of the cornea that is immediately adjacent to the limbus is spared, usually a strip of about 1-2 mm. The center of the cornea shows normal thickness, with an intact central epithelium, but the inferior cornea exhibits a peripheral band of thinning, to about 1-2 mm. The Bowman's layer of the cornea may be absent, irregular, or have ruptured areas. There may be an increase in the number of mucopolysaccharides in the corneal stroma. The thinning of the corneas may approach 20% of normal thickness. PMD is an idiopathic, non-inflammatory condition. This is described as a "beer belly" appearance since the greatest protrusion occurs below the horizontal midline (unlike keratoconus). The cornea may protrude anteriorly just above the region of thinning cornea. The distribution of the degeneration is crescent or arcuate shaped. PMD is characterized by bilateral thinning ( ectasia ) in the inferior and peripheral region of the cornea. Normally, PMD does not present with vascularization of the cornea, scarring, or any deposits of lipid. While PMD usually affects both eyes, some unilateral cases have been reported. However, in rare cases, PMD may present with sudden onset vision loss and excruciating eye pain, which occurs if the thinning of the cornea leads to perforation. Unlike keratoconus, pain is not typically present in pellucid marginal degeneration, and aside from vision loss, no symptoms accompany the condition. The term "Pellucid Marginal Degeneration" was first coined in 1957 by the ophthalmologist Schalaeppi.The word "pellucid" means clear, indicating that the corneas retain clarity in Pellucid Marginal Degeneration. It is typically characterized by a bilateral thinning ( ectasia ) in the inferior and peripheral region of the cornea, although some cases are unilateral. Pellucid Marginal Degeneration (PMD keratotorus), is a degenerative corneal condition, often confused with keratoconus.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
